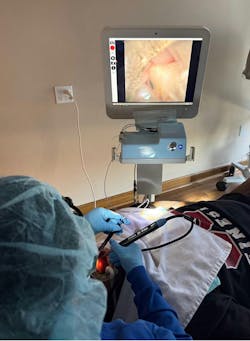
Dental endoscopy: The most underutilized technology in modern dentistry
Key Highlights
- Dentistry shouldn’t be “blind.” Just as medicine relies on advanced imaging for precision, dental endoscopy provides real-time visualization that improves diagnostic accuracy and treatment outcomes.
- Better visibility improves periodontal care. Endoscopic guidance during scaling and root planing helps clinicians detect and remove residual subgingival calculus that tactile methods often miss.
- A tool for modern, patient-centered dentistry. Dental endoscopy enhances diagnosis, supports patient education, and promotes more predictable, evidence-based care across multiple dental disciplines.
Have you ever needed a surgical procedure inside the body—heart surgery, a gastrointestinal procedure, or treatment involving a vital organ? In medicine, the first step is never to “go in blind,” but to obtain imaging that provides a clear road map. Just as critical is the use of advanced visualization technologies, often endoscopic surgery, where real-time camera guidance enhances precision, improves safety, and optimizes patient outcomes with minimal downtime.
Medicine adheres to the current standard of care; when superior technology exists, lesser approaches are not offered. This is supported throughout medical literature, which consistently shows that enhanced visualization during minimally invasive surgery improves detection of intraoperative events, reduces risk, and lowers complication rates, while poor visualization contributes to inefficiencies and adverse outcomes.1-3 As a result, surgeons across disciplines from neurosurgery to laparoscopy reject blind procedures in favor of image-guided approaches that prioritize accuracy and patient safety.1-3
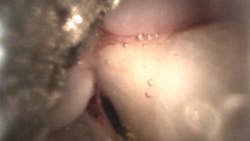
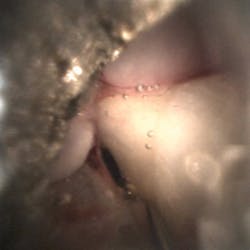
So, the question must be asked: why is dentistry treated differently? In dentistry, we have access to dental endoscopic technology that allows clinicians to visualize subgingival biofilm and calculus, perform visual periodontal therapy, identify root fractures, decay, and anatomical anomalies, and even see within root canal systems, yet many procedures are still performed without direct vision. Too often, clinicians rely on assumptions and educated guesses about what is truly happening beneath the gingival margin.
Why are we not consistently practicing to the current standard of care when real-time subgingival visualization is readily available? Greater visibility leads to more precise diagnoses, more accurate treatment planning, and more predictable clinical outcomes. Ultimately, this level of precision benefits everyone involved: patients save time, financial resources, and emotional stress, while practices reduce unnecessary appointments, avoid clinical uncertainty, and move from guesswork to confidence in prognosis and care. This article will highlight the clinical applications of dental endoscopy and its role in improving diagnostic clarity, treatment outcomes, and overall patient experience.
Clinical applications of dental endoscopy
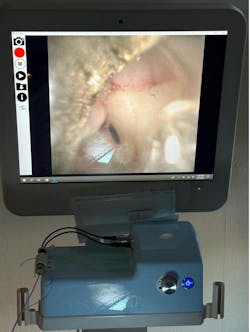
Dental endoscopy has a range of clinical applications in periodontal and diagnostic care, most notably as an adjunct to visual scaling and root planing. When utilized during nonsurgical periodontal therapy, the periodontal endoscope provides real-time magnified visualization of subgingival structures, which is not achievable through tactile evaluation or radiographs alone. This visual access facilitates the clinician’s ability to detect and remove residual calculus and biofilm more precisely, particularly in deeper probing depths and interproximal areas where tactile methods often fail to identify deposits.
Studies have demonstrated that sites treated with periodontal endoscopy have significantly less residual calculus following debridement compared with conventional scaling and root planing alone, especially in deeper pockets, indicating its utility in improving the thoroughness of nonsurgical therapy.4-6
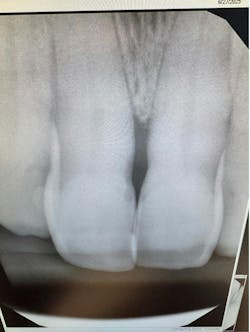
While traditional periodontal therapy is performed “blind” below the gingival margin, research shows that combining visual subgingival imaging with conventional instrumentation increases detection of calculus that would otherwise remain undetected by explorer or curette alone, supporting the role of endoscopy in improving diagnostic accuracy in periodontal care.4-6
In addition to periodontal therapy, dental endoscopy can enhance the diagnosis of subgingival caries and other structural anomalies that are not visible on radiographs or through conventional tactile exams. Visual confirmation through endoscopic imaging not only increases diagnostic precision but can also serve as a powerful patient-education tool, improving communication and treatment acceptance by allowing patients to see pathology in real time.4
Furthermore, endoscopic visualization has utility in endodontics and other disciplines where magnification and illumination improve identification of canals and anatomical complexities, evidence that enhanced intraoral visualization benefits multiple areas of dental practice beyond periodontal therapy.7
Why dental endoscopy belongs in modern practice
In contemporary dental practice, the standard of care for managing periodontal disease and complex intraoral pathology must mirror the diagnostic precision and minimally invasive principles upheld across medical disciplines. Dental endoscopy offers clinicians a level of visual insight, diagnostic accuracy, and procedural precision that is unattainable with traditional blind or tactile-only methods.
Evidence demonstrates that adjunctive use of periodontal endoscopy significantly reduces residual calculus during scaling and root planing compared with conventional approaches, particularly in probing depths greater than 5 mm, where subgingival deposits are most difficult to detect and remove.4-6
Visual access enables clinicians to confirm endpoints of debridement, identify pathoses that radiographs cannot reveal, and tailor interventions based on direct visualization rather than subjective feel.4-6
Beyond periodontal therapy, enhanced intraoral imaging supports more accurate diagnosis across a range of dental disciplines, from detecting hidden caries to identifying root canal anatomy, reducing clinical uncertainty and supporting superior patient outcomes.4,7
As dentistry evolves toward precision care and evidence-based interventions, the dental endoscope represents not merely a diagnostic tool but a clinical necessity, one that aligns periodontal therapy with the principles of modern medicine, supports patient education and treatment acceptance, and ultimately elevates the standard of oral health care. Integrating dental endoscopy into modern practice is therefore not optional; it is essential to achieving comprehensive, predictable, and patient-centered care.
Editor’s note: This article first appeared in Clinical Insights newsletter, a publication of the Endeavor Business Media Dental Group. Read more articles and subscribe.
References
- Stefanidis D, Scerbo MW, Sechrist C, Mostafavi A, Heniford BT. The importance of visualization in minimally invasive surgery. Surg Endosc. 2012;26(7):1856-1861.
- van Det MJ, Meijerink WJHJ, Hoff C, Totte ER, Pierie JPEN. Poor visualization and surgical error in minimally invasive procedures. Surg Endosc. 2010;24(7):1568-1575.
- Schwartz MS, Lin HM, Hinson H, et al. Intraoperative imaging and navigation in surgery. Ann Surg. 2018;267(2):220-226.
- Cortellini P, Tonetti MS. Clinical and radiographic outcomes of periodontal endoscopy in nonsurgical treatment of moderate and deep pockets: a 2-year randomized clinical trial. J Clin Periodontol. 2006;33(7):489-497.
- Wennström JL, Lindhe J, Nyman S. Residual calculus after debridement with or without adjunctive periodontal endoscopy: a clinical assessment. J Periodontol. 2014;85(9):1199-1206.
- Ramfjord SP, Hill RW. A comparison of residual subgingival calculus after scaling with a periodontal endoscope versus conventional scaling. J Periodontol. 2013;84(11):1605-1612.
- Moshonov J, Michaeli E, Nahlieli O. Endoscopic root canal treatment. Quintessence Int. 2009;40(9):739-744.
About the Author

Marvelyn Navarro, RDH
Marvelyn Navarro, RDH, is a dental hygienist with over 15 years of clinical and administrative experience. Her passion lies in preventive care, periodontal therapy, and addressing airway-related concerns to improve overall health outcomes. She is the founder of Perio Precise, where she specializes in periodontal endoscopy, providing advanced subgingival therapy and clinical training to hygienists across the country. A key opinion leader, national speaker, and content creator, Marvelyn serves as the current president of the Nevada Dental Hygienists’ Association.