How good communication leads to our best clinical work in dentistry
Editor’s note: The following information and clinical points are from the Dawson Academy.
I COULD SEE the hesitation and distrust in Don’s eyes when he came to my practice last year. He said, “My whole mouth hurts. I can’t get through a day or get a good night’s sleep without taking Advil.”
Don had been in pain for about six months, mainly on the lower right side of his mouth. And the pain increased when he ate hard or crunchy food. He had visited other dental professionals, but he hadn’t found relief.
I knew that I needed to build Don’s trust quickly, or I wouldn’t have a chance to address his problem and relieve him from the pain he was experiencing.
In this case, I used communication skills to gain Don’s trust, which in turn, created the opportunity to do my best clinical work to solve his issue.
Active listening builds trust
The science of dentistry is incredibly important, but sometimes the art of communication gets lost when we are too laser-focused on the clinical aspects of dentistry. Dentistry is both an art and a science, which I learned in my first dental school class at Georgetown University. But too often this lesson is lost when we focus on questions such as, “How do I make the smile line?” or “Where do I put the implant?”
Our patients want to be heard. It sounds simple, but it’s often an overlooked skill in dentistry. Active listening allows you to clearly hear your patient’s problems, fears, and past experiences.
In fact, it was the first step in the healing process for Don.
In dentistry, active listening includes the following process:
- Making eye contact. I spoke with Don while he was upright in the dental chair so that we were eye-to-eye throughout the conversation, rather than speaking to him while he was reclined in the chair—an important nonverbal tip to keep in mind.
- Paying attention when your patient is talking. Stop what you’re doing to show that you’re listening.
- Waiting until the patient is finished before responding. Don’t interrupt to ask clarifying questions.
- Verifying what you heard. Verbally summarize what you think your patient said.
All of these things will help you relay that the patient sitting in front of you is the most important person in your practice.
Do a complete exam
I walked Don through our interview process and explained how a complete exam would be an integral part of his diagnosis. The complete examination is an essential tool in the process of complete dentistry. It is a duty that we owe to all of our patients.
The complete exam allows us to:
- determine the health and position of the temporomandibular joints,
- identify the functional path of occlusion and look for occlusal instability,
- check the muscles of mastication for symptoms of disharmony,
- identify airway and health issues related to dentistry, and
- begin to recognize the cause of the patient’s problem.
The Dawson Academy’s complete exam includes the following four elements:
1. Preclinical interview—Before the examination begins, it is important that the dentist or team member conducts a preclinical interview to understand why the patient is there, past experiences, desired changes, and any occurring or reoccurring problems.
2. Restorative charting, periodontal exam, and oral cancer exam—After the preclinical exam, the dentist should identify any signs of disease within the masticatory system. To do so, the dentist should perform a restorative charting and periodontal exam to identify microorganism-induced breakdown, such as caries and periodontal disease. Additionally, the dentist should always screen for oral cancer.
3. TMJ occlusal exam—In order to fully identify signs of disease and instability in the masticatory system, dentists must also perform a TMJ occlusal exam. This exam records patient history, range of motion, centric relation load test, TMJ Doppler auscultation, muscle palpation, and an evaluation of dentition for wear, mobility, and migration.
4. Airway evaluation—Diagnosing and addressing potential airway issues is a key component in this process, as breathing issues usually need to be treated to get the patient comfortable before other treatment. Never begin building a treatment plan without understanding the patient’s airways.
It is always effective to obtain patient records—such as radiographs, CBCTs, and MRIs—to understand the patient’s dental history.
Getting to the source of the problem
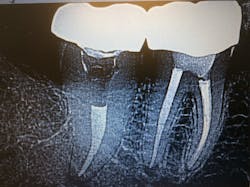
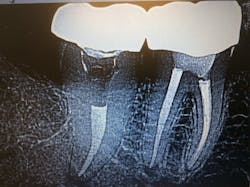
Through the complete exam and radiographs, I discovered that Don’s pain originated from tooth No. 31. The radiograph revealed an open mesial margin and periodontal ligament thickening at the apical portion of the root.
I also saw that Don had a crown done a few years ago, and he had gone back to his dentist several times for adjustments. As it turned out, the crown had an open mesial margin, which led to an undiagnosed abscess that lingered for six months (figure 1).
Next, I presented a treatment plan to Don, using similar communication strategies as in the initial conversation.
- I maintained eye contact to show that he had my attention.
- I nodded my head to show I was engaged.
- I kept an open posture and avoided crossing my arms because it can send a negative nonverbal message to the patient. I like to hold an object, such as a pen or notepad, to reinforce this habit.
- I avoided interrupting with questions.
- I summarized Don’s problems and concerns to ensure that I had all of the facts right.
- I slowed down when explaining complex information.
- I smiled. Maintaining a pleasant expression sets the tone of the conversation.
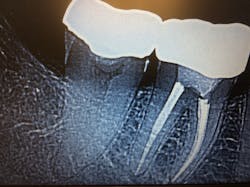
Don left my office with an antibiotic prescription and a referral to an excellent endodontist. He soon followed up with the endodontist and was successfully treated with a root canal and a new crown (figure 2).
Within a few days, he said his pain had decreased significantly, and he was finally getting a good night’s sleep. Most importantly, though, I gained Don’s trust.
Final thoughts
Effective communication lies within the art of dentistry. It is what builds trust and credibility with our patients—an essential step in the process of complete dentistry that leads to truly knowing your patient. And, it is a patient’s trust that allows us to apply our knowledge. Trust is the gateway that allows us to do our best clinical work.
Read more clinical dentistry articles at this link.
Editor's note: This article originally appeared in Breakthrough Clinical, a clinical specialties newsletter from Dental Economics and DentistryIQ.
About the Author

Joseph Rosenwald, DDS
Joseph Rosenwald, DDS, is a faculty member of the Dawson Academy, leading the Washington, DC, chapter of its Dawson Study Club. He owns and practices full time at Implant Cosmetic Dentistry in Montgomery Village, Maryland, with extensive experience in advanced restorative dentistry and TMJ disorders. Dr. Rosenwald is a member of the American Dental Association, the Academy of General Dentistry, and the American Academy of Cosmetic Dentistry. He is also a colonel in the United States Army Reserve.