Introducing the Activ GP Precision Obturation System
By Kenneth Koch, DMD, and Dennis Brave, DDS
It has been a continuing goal of Real World Endo to develop products and techniques that will deliver excellent endodontic results. It has been an additional goal to design these techniques in such a manner that the greatest majority of practitioners will be able to perform these procedures accurately and in a predictable manner. The EndoSequence file system has given all clinicians the ability to produce predictable shaping procedures that lead to synchronicity between the preparation and the master cone fit. Advancing this concept to the next level in obturation is the Activ GP Precision Obturation System (Real Word Endo/Brasseler USA, figure 1).
Activ GP is a system that utilizes new improved glass ionomer technology to create a true single cone monobloc obturation. This is very significant because a true monobloc will allow us, for the first time, to create a hermetic seal within the root canal space. A hermetic seal has been a goal of endodontics for more than 50 years. Furthermore, a true single cone technique is a method that is now achievable as a result of improved material science. An effective single cone technique will give the greatest percentage of clinicians the ability to produce superior obturation results. But, the question remains, why did we choose glass ionomer?
In our pursuit of a true monobloc single cone technique, we have felt allegiance to glass ionomer because of its superior biocompatibility and its physical properties. We have also envisioned a single cone obturation technique as one that uses a minimal amount of sealer rather than the excess that is utilized in other methods. But, more specifically, what is it that we really like about glass ionomers?
“Glass ionomer has always been our friend in dentistry.” Actually, the merits of glass ionomer are numerous. First, in addition to having the capability of wet bonding (does well in a moist environment), glass ionomer actually creates an ionic bond to the dentin. This bond is critical if we are thinking in terms of a monobloc. Secondly, glass ionomers are nonresorbable, which is critical in a single cone or sealer based obturation technique. The fact that it does not undergo resorption is not a problem with glass ionomer because of its great biocompatibility. In fact, these cements are used routinely in orthopedic surgery to hold fixtures or fragments in place. Additionally, it has also been shown in endodontic research not to undergo resorption when extruded periapically. This finding confirms its low tissue solubility.
Another aspect of glass ionomer that is preferred (especially when compared to resins) is that it responds well in the presence of sodium hypochlorite. Resins and their bonding capability are adversely affected by exposure to bleach (sodium hypochlorite). This is not a factor in restorative dentistry but becomes problematic in endodontics where we routinely use copious amounts of bleach during a root canal procedure. Webs, fins, and anastomoses are difficult, at best, to completely dry. Glass ionomer is hydrophilic and will bond to dentin in the presence of moisture.
Setting time has always been important in obturation, and the setting time of glass ionomer is such that the clinician can do a post preparation and place a post at the same visit as the endodontic procedure. When using the Activ GP sealer, there is no need to wait 45 minutes or to use a curing light in repetitive stages. This is very convenient for today’s clinician.
The Activ GP System, which is ISO-sized and -colored, is available in two types. The regular Activ GP System includes gutta percha points that are manufactured in a traditional design and impregnated with glass ionomer and subsequently coated with the same glass ionomer. The other choice, Activ GP Plus, has a different cone design. Activ GP Plus employs calibration rings for easy depth measurement and a unique barrel handle which, when placed with the insertion instrument (transporter), facilitates easy placement into the canal. The transporter is particularly handy when inserting cones into canals of posterior teeth (figures 2a, 2b, and 2c).
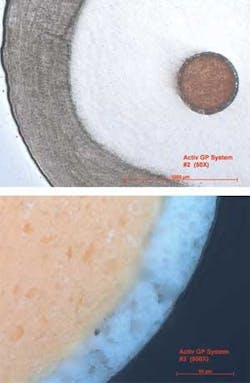
The Activ GP system has been shown to deliver a monobloc obturation result through a true single cone technique (figures 3a and 3b). Additionally, the system still remains precision-based. As mentioned in previous articles, precision-based endodontics requires accuracy between the file and the master cone. The sizes of Activ GP points are consistently accurate and are verified as such by laser measurement. In fact, all Activ GP points are laser verified to match the preparations made by the .04 or .06 tapered EndoSequence file system. The precision matching of the primary cone to the preparation is very important with a single cone technique because the accuracy of the cones to the preparation minimizes the amount of sealer and any potential shrinkage. It has been shown repeatedly that the thicker the layer of sealer, the more prone it is to dimensional change (shrinkage). Although shrinkage can occur with all sealers, glass ionomer displays the least amount of material change. Consequently, it may be stated that a true single cone technique, regardless of the material employed, should be accomplished with a constant tapered preparation such as a .04 or .06. A variable taper technique is not recommended because of the lack of precision and the increasing amount of sealer required as one progresses coronally in the canal. This lack of precision is why most variable taper preparations are associated with thermoplastic techniques. The challenges met in glass ionomer technology that allowed the Activ GP system to come to fruition are primarily associated with the sealer and the modified cone.
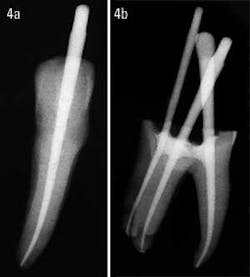
Glass ionomer cements in the past had some handling inconsistencies. Generally, the working time was not sufficient, the mix could not be altered, and the radiopacity was moderate, at best. Activ GP sealer has been modified in such a manner that, when mixed on a chilled glass slab, it will easily give a 20-minute working time. If the working time needs to be extended, simply add more liquid and mix it like zinc phosphate cement. The extra liquid is not a concern because the use of glass ionomer in a root canal is not about excessive bond strength, but rather about sealability. The radiopacity of Activ GP sealer has also been increased significantly, with the result being that the cases will not only work well, they will also look good (figures 4a and 4b).
In the past, glass ionomer did not demonstrate a bond to gutta percha. The goal of a true monobloc (and a hermetic seal) can only be achieved if we have a bond to the canal wall as well as to the primary cone. By placing glass ionomer particles into the gutta percha and then coating the cone with glass ionomer to a thickness of two microns, we now have a primary cone that will allow the glass ionomer sealer to directly bond to it. This was the key to producing a true monobloc that will work in all canal shapes.
The technique associated with Activ GP is quite simple. Following completion of your constant taper preparation and verification by X-ray of the fit of the Activ GP cone, choose a hand file that matches the final size of the preparation. The next step is to mix the sealer.
Place a half scoop of powder on a chilled glass slab and divide it into lines. Add three drops of liquid to the same slab and spatulate the powder into the liquid. The mixing technique with Activ GP sealer is very similar to zinc phosphate cement. If the consistency is a little too thick, simply add some liquid and re-spatulate.
After mixing is completed, coat the selected file with the Activ GP sealer and, with a slow circular motion, take the coated file to working length. Due to the viscosity of the sealer, we recommend that you repeat this process a second time. As in all obturation techniques, the sealer should be confined to the root canal space.
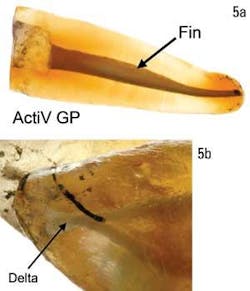
Following the placement of sealer, choose the Activ GP cone that matches the last rotary file taken to length. Coat the cone with Activ GP sealer and slowly insert it into the canal to its working length. Due to the matching size between the file and the master cone (synchronicity), hydraulics are generated which will move the sealer into lateral canals, webs, and fins (figures 5a and 5b). However, because it has been inserted slowly, any significant excess of sealer will extrude out coronally alongside the cone.
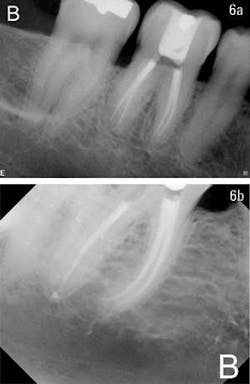
Once the cone has been inserted and verified with a digital image or X-ray, it is recommended to sear off the cone at the orifice and to remove an additional 1 to 2 millimeters of gutta percha from the canal. At this point, simply place Activ GP sealer on top of the cone to act as a canal cap. Some dental schools in North America actually recommend covering the entire chamber floor with glass ionomer to prevent leakage. This is the clinician’s choice, but it is highly recommended to place a final canal cap on top of the obturated canal. If retreatment is ever necessary, the caps are easily removed with an ultrasonic. However, if the patient loses the temporary filling, he or she has not lost the root canal. This is very important because experience has shown us that often a patient has the endodontics completed, yet has exhausted most of his or her insurance coverage for the year. Consequently, the patient walks around for a long time (up to a year) before having the tooth properly restored (figures 6a and 6b).
In this article, we have introduced to you a new obturation technique that breaks the mold of conventional methodology. It has been previously established that thermoplasticized gutta percha shrinks upon cooling. It has also been long recognized that a true room temperature single cone obturation technique would give the greatest majority of clinicians the opportunity to produce superior filling results. This has finally happened as a result of endodontic synchronicity (EndoSequence) and improved material science (Activ GP). Welcome to a new era in endodontics.
Dr. Dennis Brave is a diplomate of the American Board of Endodontics and a member of the College of Diplomates. In endodontic practice for 27 years, he was the senior managing partner of a group specialty practice. Dr. Brave, formerly an associate clinical professor at the University of Pennsylvania, currently holds a staff position at The Johns Hopkins Hospital. Dr. Kenneth Koch is the founder and past director of the program in postdoctoral endodontics at the Harvard School of Dental Medicine. In addition to having maintained a private practice limited to endodontics, he has written numerous articles on endodontics and maintains a faculty position at Harvard. They can be reached at Real World Endo at (866) 793-3636 or through www.realworldendo.com.