Considerations in dental treatment planning: Focus on revision of failed endodontic cases
When indicated, retreatment of failed endodontic treatment is efficient, safe, and predictable. Retreatment allows retention of the natural tooth. Natural tooth retention alleviates the need for extraction, implant surgery, and subsequent restoration. Depending on the study and its inclusion criteria, success rates for retreatment are generally higher than apical surgery. When taking into account costs, surgical stress, recovery time, among other variables, patients understandably favor retreatment over endodontic surgery.
RELATED |Know the tooth and know the patient: Preoperative case assessment strategies to avoid clinical dental shortcomings in endodontic treatment
While endodontic retreatment is generally a specialist procedure, assessing retreatment possibilities relative to the alternatives is central to needed treatment planning decisions of the general dentist when faced with a failed root canal. This column was written to discuss both optimizing endodontic success and as an aid in such treatment planning considerations.
RELATED |Endodontics vs. implants: understanding the possibilities of retreatment procedures -- Part 1
RELATED |Endodontics vs. implants: understanding the possibilities of retreatment procedures -- Part 2
It is axiomatic that the first attempt at root canal treatment provides the best opportunity for an optimal clinical outcome. Second attempts at treatment almost always impose some limitation onto the endodontist to one degree or another. Referral may be the best option, especially in cases of complex anatomy or patient behavioral challenges.
While clinical opinions vary as to the best way to accomplish root canal treatment, there are many different clinically acceptable methods and materials, none of which is absolutely superior to another. It is the philosophy and experience that guide the hand performing root canal treatment, not the instruments used that ultimately will create success or failure. The greatest system in the world can easily lead to clinical misadventure if placed in the wrong hands. Alternatively, even the most basic equipment kit can create a masterpiece when placed in experienced hands. Putting a novice driver behind the wheel of an Indy 500 car does not make a competitive racer.
Extrapolating, the vast majority of clinical misadventures can be foreseen and avoided with proper preoperative evaluation. Having both the correct system and methods for the particular anatomy cannot be overstated, as not all approaches are appropriate for every anatomy encountered. The philosophy that the tooth can always be retreated or referred later in the event of failure is rarely if ever productive for either the general dentist and most especially for the patient.
With this as a background, there are three primary reasons for endodontic failure, among others: uncleaned and unfilled canal space, vertical root fracture, and coronal leakage. Of these three mechanisms of failures, the clinician has, for the most part, a large degree of control over each. Use of the rubber dam, visualization and magnification (ideally through a surgical operating microscope), straight-line access, identification of all canals, achievement and maintenance of patency, three-dimensional cleaning, shaping, and obturation, and placement of a coronal seal can lead to very high levels of clinical success — 95% or greater — thus eliminating a scenario that later requires considering retreatment.
An intangible yet critical aspect of attaining endodontic success that is little discussed is the patient’s degree of cooperation and phobia and/or physical limitations imposed by the clinical scenario (patient cannot be reclined, is in a wheelchair, has a limited opening, the tooth is tipped, rotated, etc). While a comprehensive discussion of this subject is beyond the scope of this article, fear and anxiety over dental treatment is a reality every day in endodontic offices around the world. Even in the best hands, many patients have varying degrees of anxiety that limit their cooperation. While there are coping mechanisms to deal with such anxiety (oral and IV sedation, nitrous oxide, profound local anesthetic, TLC, and compassion, etc.), some percentage of endodontic procedures will be done under adverse circumstances. Regardless of the good intentions, compassion, and skill of the clinician, some percentage of these clinical situations will impact the final quality of the treatment. Optimizing results requires the clinician to consider these challenges preoperatively and make appropriate decisions in patient management.
As an aside, given the above, it is important never to criticize the treatment of a fellow dentist. Just looking at the radiographic image, it is not possible to know under what circumstances the treatment was performed. In fact, what might appear to be substandard treatment on the film may be a relative masterpiece given the limitations imposed by the patient or the situation. Except in the case of malpractice, if we were not there to see the treatment, if is not fair to judge the outcome, all things being equal.
The above considerations notwithstanding, if endodontic failure occurs, assessing the possibilities for retreatment of failed root canal treatment is an essential skill. Assessment of restorability and periodontal status is a key starting point. Multiple radiographic angles (as well as a CBCT image if indicated) can go far to alert the clinician to the reasons for clinical failure (missed canals and uncleaned and unfilled canal space, vertical fracture and coronal leakage, etc). In my clinical experience, virtually every crown I have accessed in retreatment has shown overt signs of coronal leakage. Even if the radiographic image of the treatment appears ideal, coronal leakage should not be ruled out as a cause of failure. In any event, the previous treatment should also be evaluated for iatrogenic events and signs of inadequate cleaning and shaping (missed canals, obturation short of the apex, etc.) in addition to the entities above.
Once the above are considered, the key decision point in feasibility of retreatment vs. extraction is the ability of the endodontist or treating clinician to remove the existing filling material without causing or exacerbating an iatrogenic event, reestablish and maintain patency, reshape the canal to the most ideal dimensions possible, disinfect and obturate the canal system, and place a coronal seal and restore the tooth to optimal functionality and esthetics.
A discussion of the armamentarium and techniques to perform retreatment are extensive and well beyond the scope of this article. But one critical technique in the above list merits special attention as it is at the heart of all retreatment procedures: establishment and maintenance of patency. New and large numbers of stainless steel hand files are required in retreatment. Stainless steel hand files are a commodity and should only be used once for this and any clinical purpose.
Appropriate use of hand K files and possibly hand files designed especially for calcified canals (for example, Mani K files and Mani D Finders respectfully) cannot be overstated in their importance for this purpose. Hand files used to gain patency are generally precurved and inserted in numerous directions until either the blockage and/or ledge (among other canal transportations) encountered can be bypassed. Regaining patency requires patience and skill, as many iatrogenic canal transportations can be made worse with indiscriminant hand file use. Caution, experience, and clinical judgment are advised.
In summary, it is axiomatic that once the financial interest of the clinician is removed from the treatment planning rationale, there are few clinical situations where extraction and implant therapy or retreatment are equally indicated. If clinicians are honest with themselves (and take their financial interest out of the equation) when making treatment planning decisions for or against retreatment vs. extraction, one treatment (performed in the best hands available) is generally indicated and in the patient’s best interest. I welcome your feedback.
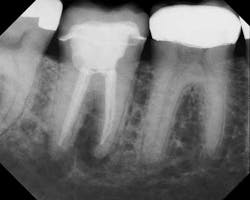
Preop
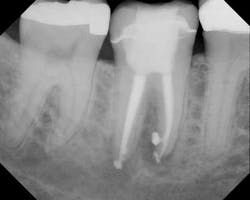
Postop