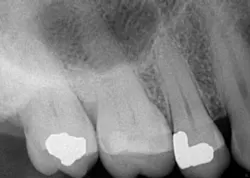
We can't save them all: the missing endodontic diagnosis
In a perfect dental world, we would like say we could save everybody’s teeth from the ultimate demise — extraction.
But our valiant attempts are often impeded by a patient’s lack of motivation, home care, or financial reasons. It is frustrating though when we go through the efforts of doing all that we know how, using all the available technology, the patient is willing and able, and we still can’t save a tooth.
ALSO BY DR. STACEY SIMMONS |Your diagnosis, please! The case of the unknown oral pathology
Such is the case for the patient who presented with a chief complaint of biting and occasional slight cold sensitivity on his upper right back molar (No. 2). The patient stated that it hurt to chew and that he wanted to get his tooth fixed as soon as possible. Upon radiographical examination, the periapical for No. 2 was normal. Clinically, the tooth presented with a conservative occlusal amalgam with caries distal to the restoration. In addition, a fracture line on the mesial and distal marginal ridges was noted. Percussion and cold testing were normal and periodontally, the tooth was stable. Bite assessment with the tooth sleuth revealed a positive response on the lingual cusp when biting and releasing. Diagnosis: reversible pulpitis secondary to a crack.
Due to the separation of the buccal and lingual cusps, a crown was recommended to restore the tooth to full form and function. In addition, the patient was informed that the fracture line likely extended further than the naked eye could observe; excavation of the tooth would reveal more detail. (1)
ALSO BY DR. STACEY SIMMONS |Quick tips on how to be a better clinical provider within all disciplines of dentistry
At the crown appointment, the amalgam filling and compromised mesial and distal marginal ridges were removed. The fracture line was indeed detected and noted to extend across the floor in a mesial/distal fashion.Fig. 3
The entire area was cleaned out, a build-up was placed, and the tooth was prepped for a full zirconia crown. At the end of the appointment, the patient was shown the picture of the fracture line and was informed that even though the tooth did not present in an irreversible nature, it still could need a root canal in the unforeseen future.
While in the temporary, the patient acknowledged that the tooth felt fine and there was no pain. The final crown was cemented and the patient was again informed of the potential for the tooth to go irreversible.
Three months later, the patient presented back with the complaint that over the course of three to four days, his tooth had progressively become more and more painful to cold, biting, and overall pressure. Percussion, biting, and palpation were sensitive and outside the range of WNL. Cold testing was vague. It is worthwhile to mention that the literature supports that when testing the vitality of a tooth, the positive predictive value (i.e., a positive result in a diseased tooth) for cold testing is 89%. (2) Given the aforementioned history of the tooth, a referral to an endodontist was recommended.
The endodontist evaluated the tooth and diagnosed the tooth with pulpal necrosis and symptomatic apical periodontitis and recommended RCT. When access was gained, the endodontist observed a necrotic pulp. Staining also showed that the crack line extended across the entire pulpal floor and down the mesial and distal sides of the pulpal cavity. Concerns with this defect included:
- The tooth, if restored, could be stable for a period of time, but a crack of this magnitude is an arena for bacteria to colonize, which would ultimately lead to failure.
- A periodontal defect could form in the furcation area from the harbored bacteria in the crack.
- Despite crown placement, biting and grinding forces could continue to exacerbate any micro-movement and again, lead to failure.
For these reasons, the tooth was given a poor prognosis and recommended for extraction. It was surgically removed, and the patient is now in the process of implant consultation and subsequent placement to restore missing function.
The cracked tooth is one of the more frustrating situations for all providers. The American Association of Endodontists has made available publications that can help with the definitions of cracked teeth and treatment options available. This can be found here.
Closure to this situation (for provider and patient) was gained through the knowledge that protocol was followed, written and photographic documentation recorded progress, and the specialist was consulted. Even via attempted heroics, we can’t save all the teeth we want to despite available resources. There are times when alternative treatment options offer a better long-term prognosis (function and financial) for the patient. Knowing when to “throw in the towel” does not mean we are incompetent or lacking in skill; it ultimately signifies that we are putting the patient’s best interests first.
The author would like to recognize Joe Petrino, DDS, MS (of Missoula, MT) as a contributor to this clinical case and for write-up consultation.
References
1. Endodontics Colleagues for Excellence. Cracking the Cracked Tooth Code: Detection and Treatment of Various Longitudinal Tooth Fractures. Summer 2008.
2. Peterson K, Soderstrom C, Kiani-Anaraki M, Ltvy G. Evaluation of the ability of thermal and electrical tests to register pulp vitality. Endod Dent Traumatol 1999;15:127-131.