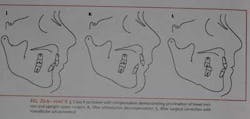
Consideration of nonsurgical compromises in Class II orthodontic cases
In the general population’s eyes, if an individual undergoes orthodontic care and has straight teeth when all is said and done, then the work of an orthodontist is considered a success. However, in the enthusiasm and focus to correct and achieve the perfect dental occlusion, there are often compromises in other areas that are not in the patient’s best interest.
ALSO BY DR. STACEY SIMMONS |Impacted canines and orthodontic treatment
Skeletal Class II problems are due to mandibular deficiency or downward-backward rotation of the mandible caused by excessive vertical growth of the maxilla. (1) When a skeletal Class II patient presents with the request to have his or her teeth aligned, the following factors must be considered:
- Is there anymore growth potential?
- What is the nasolabial angle, and what does the facial profile look like?
- What are the options to correct malocclusion?
- What benefits does mandibular advancement surgery offer?
- If extraction is a consideration, is there a trade-off or compromise?
ALSO BY DR. STACEY SIMMONS | Braces: the good, the bad, and the ugly
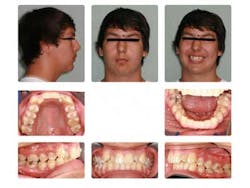
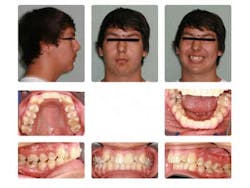
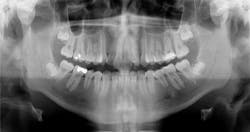
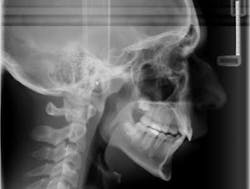
Case report A healthy 16-year-old male presents with Class II bite, an obtuse nasolabial angle, a slight, long concave profile with deficiency in the growth of the mandible, and inadequate spacing for the maxillary teeth. What are the options and talking points for this treatment plan?1. There is likely very little growth potential left in this patient, so trying to capture any remaining growth would be minimal.
2. If we were to focus only on the occlusion (minus profile, etc.), then it would be simple to extract the maxillary 4’s (1st bicuspids) and then acquire a somewhat ideal alignment of the arches.
3. In reference to point No. 2, orthodontic treatment planned without mandibular jaw advancement surgery in these types of cases generally will build in more dental compensations for skeletal variation (2), as the profile is compromised even more with a wider nasolabial angle, longer profile, and thus limiting the ability for any future facial profile correction.
4. The ideal treatment and recommendation would be to perform a lower jaw advancement surgery to give an ideal position of skeletal and dental components. Worms et al. reported that the total interrelationships of surgical and orthodontic contributions are in the best care and interest of the patient long term. (2)
5. It can be argued that mandibular jaw advancement surgery could, down the road, cause TMJ concerns/issues or create a dual bite. A study done by Mihalik et al. reported that orthodontics-only patients reported fewer functional or TMJ problems than did the surgery patients, but patients who had their mandibles advanced were significantly more positive about their dentofacial images. (1) This is an important concept to remember — beauty is in the eye of the beholder!
6. If surgery is not an option or desired at that time, then many would consider again not to extract the upper 4’s and use a functional appliance, such as a Herbst to attempt to advance the mandible while aligning the teeth as best as possible. In the end, however, there would likely be excess overjet of the anterior teeth in this type of compromise.
It could be concluded with the aforementioned talking points that there is not a right or wrong way to proceed in cases like this. Some options are better than others, but this is the take-home point: If a Class II patient (as presented herein) does have the upper 4’s removed, it exacerbates the existing profile and limits virtually any potential for a correction of profile in the future. It is, therefore, vital to discuss all risks, benefits, complications, and alternatives so the patient can make the best decision possible. Assuming no regard to cost or possible complications, the mandibular advancement would be considered by most to be the preferential treatment in this case, as it resolves the core problem — mandibular deficiency. In this case, the patient was not willing to undergo a surgical procedure at this time, so the treating orthodontist advised the family against the removal of maxillary teeth in order to preserve facial profile and allow for possible future mandibular advancement procedure.
Acknowledgements: The author would like to recognize Dr. Padraig Dennehy for his insight to the write-up and case report. He can be reached by email at [email protected]. Visit his website at www.dennehyorthodontics.com.
References
1. Mihalik CA, Proffit WR, Phillips C. Long-term follow-up of Class II adults treated with orthodontic camouflage: A comparison with orthognathic surgery outcomes. American Journal of Orthodontics and Dentofaical Orthopedics. Mar. 2003; 123(3):266-278.
2. Worms FW, Isaacson RJ, Speidel TM. Surgical orthodontic treatment planning: Profile analysis and mandibular surgery. The Angle Orthodontist: An International Journal of Orthodontics and Dentofacial Orthopedics. Jan. 1976: 46(1).
3. Contemporary Oral and Maxillofacial Surgery, 4th Edition. Peterson, Ellis, Hupp and Tucker. 2003. St. Louis, Missouri. Mosby.
About the Author
Stacey L. Simmons, DDS
Editorial Director of DE's Breakthrough Clinical e-newsletter
Dr. Stacey Simmons grew up in Hamilton, Montana. She did part of her undergraduate work at Purdue University and then received her bachelor’s degree in exercise physiology from the University of Utah. After applying to both medical and dental school, she decided that dentistry was her career of choice. She received her DDS degree from Marquette University School of Dentistry in Milwaukee, Wisconsin, in 2004. In private practice, she focuses her care on prosthodontics and cosmetic dentistry. She is a guest lecturer in the Anatomy and Physiology Department at the University of Montana. Outside the office, she trains for triathlons and spends time with her family. You may contact Dr. Simmons by email at [email protected].
In 2015, Dr. Simmons became the editorial director of DE's Breakthrough Clinical with Stacey Simmons, DDS, an e-newsletter focused on breaking through plateaus in clinical practice. Subscription information may be found here.
Updated May 4, 2016