Silver diamine fluoride: A dental hygienist's perspective on the latest protocol for high-risk patients
Judy Zack Bendit, RDH, BS, shares her perspective on silver diamine fluoride as a protocol for high-risk dental patients. Read about how she used it on a recent mission trip, its indications and contraindications, what to know if you plan to use it in your practice, her procedure for using it, and finally, what code to use for documentation and billing.
For many years, I heard about a product called silver diamine fluoride, but it was not available in the United States. That changed in August 2014 after it was approved by the Food and Drug Administration (FDA) and launched at the American Academy of Pediatric Dentistry (AAPD) meeting in April 2015.
Silver diamine is not new to the world—just to the United States. Researchers around the world have been working with silver nitrate and silver diamine for years, both in medicine and dentistry. In 2009, Rosenblatt, et al., coined it "the silver-fluoride bullet." (1) Elevate Oral Care brought this product to market in the United States as Advantage Arrest silver diamine fluoride 38%, and it is something you need to know about. It contains a solution of 5% fluoride, 25% silver, and 8% ammonia: The fluoride promotes remineralization, the silver acts as an antimicrobial, and the ammonia stabilizes the ingredients in the solution. Its clearance from the FDA is identical to that of fluoride varnish, but off-label use is where we will see some exciting new protocols for high-risk patients.
My mission trip
I was excited to bring a bottle of silver diamine fluoride on a mission trip to the Dominican Republic, where I spent a week with 24 dental students from Nova Southeastern Dental School. I typically do one to two mission trips each year, focusing on cleft lip and palate patients and community outreach, so this was a new experience. Instead of doing all of the work, I was there as a faculty member to facilitate and oversee the work done by the students. Before going, I read all of the articles I could find that had been written about silver diamine fluoride and spent a few hours with Jason Hirsch, DMD, a pediatric dentist in south Florida who uses the product on a daily basis. I was excited to teach the students about this "hot" new procedure.
We painted 140 tooth surfaces with silver diamine fluoride, and the results were outstanding. The students found the material easy to use since it only took seconds to place and did not require air and water. They loved the fact that patients could eat or drink immediately afterward and the fact that the procedure did not require any anesthesia or drilling to prep the tooth. Because the fluoride component of silver diamine fluoride is two times greater than that of a typical varnish treatment, no additional fluoride varnish treatment was necessary because the fluoride would precipitate in the saliva and work the same way a traditional treatment would. We placed silver diamine fluoride for very young patients as well as for older patients with severe recession and root caries. It allowed us to treat many more patients than we would have under normal circumstances.
Why you should consider it
Silver diamine fluoride has been shown to arrest decay, so it allows us to control the pain and infection with less trauma. As I mentioned above, it's easy to use and takes seconds to apply. It's noninvasive; with no need for sedation or local anesthesia, it's less traumatic for children. And it's affordable—each bottle dispenses 250 drops of solution, and each drop will cover five surfaces.
Indications
Silver diamine fluoride can be used for patients who are at an extreme risk for caries, from severe early childhood caries to severe adult root caries. Those of you who work with behavioral and medical management patients should also consider using it. Consider silver diamine fluoride for patients with limited access to care and nursing home patients, as well as for posterior restorations, under restorations, and to save existing restorations. Think about a restoration that is starting to leak or that is otherwise becoming compromised; silver diamine fluoride can be used to protect the tooth from hidden caries. It can potentially help us avoid taking patients to the OR for treatment.
Contraindications
An allergy to silver is the main contraindication. Do not use silver diamine fluoride for patients who present with ulcerative gingivitis and stomatitis. Also, silver diamine fluoride is not indicated if there is pulpal involvement.
Considerations
If esthetics are an important consideration, silver diamine fluoride should not be your product of choice. It turns the decay from brown to black, and to date, we don't have a restorative product that will completely mask the discoloration.
Be careful when working with this material. If it touches skin, it leaves a stain like a temporary tattoo, which disappears within a few weeks. Silver diamine fluoride can also stain clothes and operatory surfaces, so be careful and use an assistant when possible.
Some clinicians may feel it's necessary to provide a second or third treatment. Because of our circumstances on the mission trip, we were only able to do one treatment per patient. Hopefully, we will be able to go back to the same area next year and see some of our patients to reevaluate them.
The American Academy of Pediatrics (AAP) and AAPD have discussed educating pediatricians about silver diamine fluoride because pediatricians look into children's mouths to see their tonsils. If they observe discoloration, they might not know what they are looking at. If your office implements silver diamine fluoride, I suggest you let the local pediatricians know about this procedure.
Procedure
In most states, silver diamine fluoride is treated the same as a fluoride varnish, so both dentists and dental hygienists can place it, but check with your state practice act to be sure.
This is how I use the product (others may use it slightly differently):
1. Wear standard personal protective equipment (PPE), and make sure the patient is wearing safety glasses and plastic-lined bib.
2. Dispense one to two drops of silver diamine fluoride into a plastic dappen dish, depending on how many teeth you are treating. One drop will treat five surfaces.
3. Apply scented lip balm to the patient's lips to help mask the smell of the silver diamine fluoride as it is placed in the mouth.
4. Use a saliva ejector when possible.
5. Isolate the tongue and cheek from the affected teeth using gauze or cotton rolls. Absorbent triangles work well.
6. Consider applying petroleum jelly to proximal gingival tissue with a cotton applicator for safety. This could help to prevent staining of the gingiva if the silver diamine fluoride touches it.
7. Dry affected tooth surfaces with air or a cotton swab.
8. Immerse a microbrush into the solution in your dappen dish and remove any excess on the side of the well. This is best done with a dental assistant to avoid spilling.
9. Apply it directly onto the affected tooth surface(s) with the microbrush.
10. Allow the silver diamine fluoride to absorb for up to one minute if possible.
11. Remove the excess with gauze, a cotton roll, or a cotton-tip applicator.
11. Rinse with water.
12. Invert all used cotton, the microbrush, and the dappen dish into a glove so it can't drip on any surface or skin. Dispose of it in a trash can.
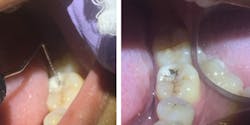
Silver diamine fluoride is applied to occlusal decay.
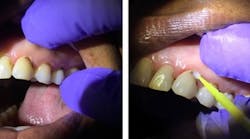
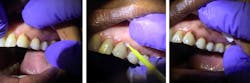
Silver diamine fluoride is applied to root decay (click to enlarge).
Silver-modified atraumatic restorative treatment (SMART)
Dr. Jason Hirsch has completely embraced this new technology. He told me very succinctly, "This is not cosmetic dentistry." When using silver diamine fluoride, it leaves a "black scar" on the tooth, but it could revolutionize dentistry. He also said, "Our kids do not have to be as traumatized as we may have been as kids."
Instead of providing atraumatic restorative treatment, or ART, he and others are providing what they call SMART, or silver-modified atraumatic restorative treatment. After arresting the decay, he restores the tooth with a self-curing glass ionomer, as some clinicians are concerned that using a light-cured composite could accelerate the black staining because of the silver component in the varnish.
Documentation and billing
D1354, a new code for "interim caries-arresting medication application," was approved by the Code on Dental Procedures and Nomenclature (CDT) Code Maintenance Commission for 2016. The code definition is: "Conservative treatment of an active, nonsymptomatic carious lesion by topical application of a caries-arresting or -inhibiting medicament and without mechanical removal of sound tooth structure."
Additional reading
In January 2016, the Journal of the California Dental Association published an article, entitled "UCSF protocol for caries arrest using silver diamine fluoride: Rationale, indications, and consent." (i) The authors review the history of silver diamine, describe a protocol for using it, and more. The article is worth reading!
Editor's Note: This article first appeared in Pearls for Your Practice: The Hygiene Product Navigator. Click here to subscribe. Click here to submit a products article for consideration.
Note
i. Horst JA, Ellenikiotis H, UCSF Silver Caries Arrest Committee, Milgrom P. UCSF protocol for caries arrest using silver diamine fluoride: Rationale, indications, and consent. J Calif Dent Assoc. 2016;44(1):17–28.
Reference
1. Rosenblatt A, Stamford TC, Niederman R. Silver diamine fluoride: A caries "silver-fluoride bullet." J Dent Res. 2009;88(2):116–125.