Staying ahead of the grim reaper: Oral cancer screening tools can help save lives
Trish Jones, RDH, BS, shares a personal account, offers statistics on the prevalence of and risk factors for oral cancer, and identifies numerous examples of adjunctive oral cancer screening tools—including light-based devices, a brush test, and a salivary test—that can enhance dental professionals' abilities to accurately screen patients for oral cancer.
As dental professionals, we sometimes take for granted what we see or what patients go through until it hits home—that is, until we become subject to it ourselves . . . More on that in a bit.
In 2014, while attending the Annual American Academy of Cosmetic Dentistry Scientific Session in Florida, I had the opportunity to listen to Ms. Eva Grayzel. She is a nationally known storyteller who is a survivor of oral cancer. With an advanced stage of oral cancer, she was given only a 15% chance of survival. She told her heart-wrenching story of diagnosis: When she was 33 in 1998, an ulcer on her tongue became larger and then painful. She described in detail how her tongue was partially reconstructed and how she had a modified radical neck dissection and radiation therapy. She brought the room full of dentists, dental assistants, dental hygienists, and guests to tears and to their feet as she spoke about her second chance at life. She was remarkable—so remarkable that her lecture left an impact on me (and, I am sure, many others) about the importance of doing an oral cancer exam on every dental patient.
According to the National Institutes of Health, oral cancer is the sixth most common cancer in the world. The disease is diagnosed in more than 45,000 American patients per year, and more than 8,000 of those patients die per year. This amounts to approximately one death for every hour of every single day each year.
_______________________________________________________________________
The 411 on oral cancer
Detecting oral cancer early can increase the survival rate to 80%–90%. Right now, the five-year survival rate of those who are diagnosed is approximately 65%, according to the American Dental Association. Detection is crucial because even the smallest asymptomatic lesions may have the potential to be malignant.
Oral cancer involving the tongue accounts for approximately 20%–25% of cases diagnosed. 15% of cases involve the floor of the mouth, 10%–15% involve the lips, and 10%–15% involve the minor salivary glands.
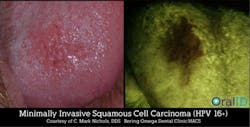
90% of oral cancers are squamous cell carcinoma, which is malignant and tends to spread quickly. Cancer that arises from the squamous epithelium can metastasize to lymph nodes and other sites—so the earlier a cancerous lesion is detected, the less chance it has had to spread.
Cancer stages indicate how far the lesion has invaded the oral cavity, as well as the severity and prognosis. The TNM staging system is used to stage cancer; it is based on tumor size and invasion level (T), the involvement of lymph nodes (N), and metastasis of the cancer (M).
Cancer Stages
Stage I:
- Lesion is less than two centimeters
- No lymph nodes involved
Stage II:
- Lesion is between two and four centimeters
- No lymph nodes involved
Stage III:
- Lesion is four centimeters or more; no lymph nodes involved
- Lesion is any size; one lymph node involved on same side
Stage IV:
- Lesion has metastasized to surrounding tissues; lymph nodes may be involved
- Lesion has metastasized to more lymph nodes to either one side or both sides of the neck
Recurrent:
- Recurrence of cancer after treatment
Since oral cancer is diagnosed routinely in later stages in development, prognosis is grim. Patients may not notice because they feel no pain, and they may not recognize symptoms to be abnormal. As dental professionals, we should make our patients aware of the facts about this cancer. Dental appointments are not just for evaluating teeth and gums. Oral cancer screenings can save lives.
Universal guidelines
Surprisingly, no mandatory universal guidelines exist for oral cancer screening programs in dental offices. Individual offices determine whether oral cancer screening is part of their protocols and whether it is done with a manual exam for abnormalities, with a device, and/or with a salivary test. These screening techniques can detect abnormalities in tissue to indicate whether further testing, such as a biopsy, is required for a definitive diagnosis. Whether to charge for screening is often left to the office’s discretion. But screenings, according to the Centers for Disease Control (CDC), should be performed on anyone over the age of 17. Why? Human papillomavirus (HPV) is spread easily, and it's the fastest-growing risk factor for oral cancer.
Risk factors
What are the risk factors for oral cancer? The most recognized risk factor is tobacco usage—including cigarettes, pipe tobacco, and chewing tobacco. Another risk factor is alcohol consumption, which is a contributing risk factor for esophageal squamous cell carcinoma. In addition, people who inherit a deficiency in an enzyme that metabolizes alcohol have been found to have a substantially increased risk of alcohol-related esophageal squamous cell carcinoma. Risk factors increase tremendously when alcohol and tobacco usage are combined.
A more recently recognized critical risk factor is HPV, which has over 170 strains and is spread through sexual contact. HPV is linked to the increase in oral cancer in nonsmokers, and it accounts for 25% of all cancers in the mouth and oropharynx. HPV and oral cancer have increased by 225% in the past three decades.
Finally, age and sex are also risk factors. Oral cancer is twice as common in men as woman, which is often considered to be due to men being more likely to smoke and/or drink. Those over 40 are at higher risk for oral cancer, although the younger generation is at a growing risk due to HPV. No one is safe.
___________________________________________________________________________
The hygiene appointment
It can’t be said enough: Oral cancer kills approximately one American every hour. Think of it this way: For each patient you see for an hour, another person will have passed away from oral cancer. The dental hygiene appointment is often the best opportunity for performing an oral cancer screening exam. The registered dental hygienist has been trained and educated to assess any abnormalities in tissue in the head and neck region. Any suspicious areas can be brought to the dentist's attention for further discussion and evaluation.
There are different kinds of screenings that can be done, such as a hands-on conventional exam that includes a visual examination of the soft tissues of the mouth, a tongue exam that involves extending the tongue to the base, and manual palpation of the cheeks, lips, gums, and borders of the tongue. The lymph nodes in the head and neck region should be palpated as they can be key in identifying the first signs of oral cancer.
___________________________________________________________________________
Diagnostic aids and the screening process
Since many lesions are not visible to the naked eye, diagnostic aids, such as fluorescence devices and salivary tests, can be useful in assisting dental professionals. Light-based systems use tissue reflectance and fluorescence to enhance the oral screening exam. One category of light-based systems uses light and dyes to assess the oral cavity, whereas the other category only uses fluorescence light to detect abnormalities. Fluorescence devices are particularly sensitive to dysplasia and cancer but can also be sensitive to vascular normal tissues. Dental professionals should be familiar with the normal appearance and patterns of oral cavity fluorescence for abnormal patterns to be more easily detectable.
ViziLite Plus from DenMat
Using incandescent light, the ViziLite Plus (DenMat) uses "TBlue" (Zila tolonium chloride) as a marker for abnormal suspicious lesions. The system also uses disposable technology to eliminate cross contamination. Basically, the patient rinses with the solution and waits five minutes. Then, in a dimmed operatory the the dental clinician uses the Vizilite Plus to identify any suspicious areas.
Microlux DL from AdDent
With the Microlux DL (AdDent), a simple mouth rinse is used first. Then, a chemiluminescent light is used to reveal any abnormal tissue, even if it is not visible to the naked eye. Microlux DL is similar to proven early detection procedures for other cancers, such as the mammogram, the Pap smear, and the prostate-specific antigen (PSA) test. The Microlux DL exam is recommended to be performed annually.
VELscope Vx from LED Dental
The VELscope Vx (LED Dental) uses tissue fluorescence, rather than reflectance. As a handheld device, the VELscope Vx system enhances visualization of mucosal abnormalities, such as oral cancer and premalignant dysplasia. This system does not require any dyes. VELscope Vx examinations are performed during routine hygiene exams under normal lighting conditions. Photo documentation is easy integrate and to share with patients or other dental specialists.
OralID from Forward Science Technologies
This system uses fluorescence technology in the form of a blue light that allows a clinician to identify oral cancer, precancer, and other abnormal lesions at an earlier stage. The battery-operated, handheld device emits a visible blue light (435–460 nm) directly into the oral cavity. Included is protective eyewear that enhances the visual effects of the blue light during the oral exam. When the blue light shines on healthy oral tissue, it fluoresces green. However, when it shines on abnormal tissue, it appears dark, due to a lack of fluorescence. With no disposables due to its unique design (like a flashlight), it is an affordable choice with product training for the team included.
BrushTest (also known as the OralCDx Brush Biopsy) from CDx Diagnostics
The BrushTest (CDx Diagnostics) is an in-office test that helps determine if white or red spots are harmless. This system consists of a specially designed brush that is used to painlessly obtain a sample of the lesion in question. The superficial, intermediate, and basal layers of the epithelium are sampled using the brush. No anesthesia is required, and the procedure is comfortable with minimal or no bleeding. The sample is sent to a specialized laboratory to be analyzed. It has been indicated that this type of testing is highly accurate.
Salimark OSCC Salivary Diagnostic Test from PeriRx
The Salimark OSCC Salivary Diagnostic Test (PeriRx) is indicated for usage when a suspicious lesion or an abnormality in the tissue is detected during visual examination and/or a fluorescence exam. The painless saliva test is the first commercial saliva test for early detection of oral squamous cell carcinoma. This system uses biomarkers in saliva that reflect cancer activity.
Which system should you get?
Which system is right for your office? The one that you are going to use! If you are uncertain about which one to incorporate into your practice, contact the companies and request additional information or a demo. (This article only mentions these products as examples.)
The oral cancer screening systems are only tools for screening and are not designed to diagnose oral cancer. False negatives can result if these products are not used appropriately. Regardless, if you choose to use one of these adjuncts, remember that the ideal screening is a conventional visual and tactile oral exam at the dental office.
What is a suspicious lesion? What if you find something?
What are you looking for? As a dental professional, you are looking for any abnormal lesions such as leukoplakia or erythroplakia. Symptoms that the patient can bring to your attention can include a sore that doesn’t heal, red or white patches, and/or pain or tenderness in the mouth or lips. The patient can also indicate whether he or she has issues with the tongue in chewing, speaking, or moving the jaw. The patient may have pain or swelling in the temporomandibular joint area or difficulty with occlusion. The patient may indicate that he or she has bad breath or abnormal taste or that he or she experiences numbness or unusual bleeding.
If any abnormality is identified, a biopsy will usually be indicated. A small sample of the tissue will be cut out or aspirated with a fine needle. It may require referral to a specialist if the area is deeper into the throat or mouth. Once a pathologist examines the tissue, results will indicate if it is cancerous and, if so, what kind of cancer it is.
Treatment of cancerous lesions usually involves surgery, but this depends on the stage and location of the cancer. Surgery may be followed by radiation or radiation in combination with chemotherapy. In advanced cases, treatment is not always successful. Up to 70% of the cases recur and can result in death. The outcomes are more positive if the lesion is diagnosed early. Sadly, symptoms and physical findings are often ignored, and most oral cancers are diagnosed at a late stage.
Charging for oral cancer screenings
To charge or not to charge? It is up to the discretion of the dentist. But if you are providing a service that may save someone’s life, it may be feasible to charge for life-saving services. The CDT code D0480 can be used for an adjunctive prediagnostic test that aids in detection of mucosal abnormalities including premalignant and malignant lesions, not to include cytology or biopsy procedures. Other codes are indicated for hard and soft tissue biopsies.
___________________________________________________________________________
Reality check
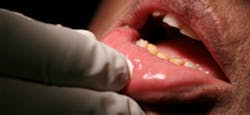
A view inside the mouth while the OralID is in use (left); Stephanie Showalter, RDH, examines the author with the OralID device at New Horizons Dental Care (right)
I recently had a reality check. At my regular dental office, my hygienist used the VELscope Vx during a routine oral cancer exam a few months ago. It showed a suspicious lesion on the left side of my soft palate. I basically ignored it, until now. I am not in pain and it doesn’t bother me. Sound like a typical patient, don’t I? Why do we think it has to be painful before we do something about it? Recently, I had access to the OralID device, and it also showed the spot on the back of my throat. Do I feel frightened now? Yes, I do. The OralID device comes with a yellow adapter for a smartphone camera, so a photo can be taken with it. This provides a constant visual for me. Yes, I have an appointment to have a biopsy because I have too much life left to live.
Oral cancer is not something to mess around with. It is a serious disease, and it is growing, due to the prevalence of HPV. With the rise of oral cancer, it is optimal to perform an oral cancer screening exam on patients on a routine basis. An exam during the hygiene appointment is an added value that can save someone’s life. A visual and tactile exam should be the basis, but adding a diagnostic detection device will enhance your ability to accurately assess patients for oral cancer, and it will make the dental office more high-tech. Save a life—provide an oral cancer screening exam for every patient at least once a year, and help keep the grim reaper away.
References available upon request.
Trish Jones, RDH, BS, is an international speaker and author with experience in esthetic dentistry, dental sales, and working in a dental laboratory. She is a past chair for the American Academy of Cosmetic Dentistry Charitable Foundation Give Back a Smile. She can be reached via email at [email protected].