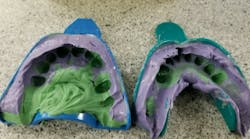
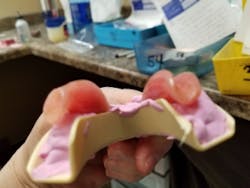
From chair to lab: Things dentists do that make lab techs' jobs more challenging
There are certain kinds of Post-it notes that I don’t like getting on my desk, and some of my least favorites are the ones with messages like this: “CALL THE LAB...they have a question about Mr. Henry’s crown/bridge/denture/implant case.” Unless I specifically tell the lab to call me (so I can clarify something that is difficult to get across in writing), those darn Post-it notes usually mean that something is not quite right with what I sent them and it needs to be redone.
Or, how about this: I go to seat a crown and the margin falls short on the radiograph. My gut instinct is to blame it on the lab (pathetic!), when in reality, it’s my fault...but I’m not going to admit that to the patient, now am I? It’s in our human nature to want to look good, and when patients are paying for our services and expertise, we want to deliver.
Let's flip the scenario around. The lab receives a case from you (an impression or scan) and your instructions are typical: “Please fabricate full zirconia crown No. 3, or immediate denture...etc.” OK, that’s easy. As the lab technician looks at what you've sent, he or she sighs and thinks, “Not another one...”
I’ll submit that as doctors it’s easy to get caught up in our daily routine—it’s what we do! What we fail to realize, however, is that on occasion we need to put ourselves in the shoes of the other people on our team—assistants, front desk, insurance/finance coordinators, hygienists, equipment and supply reps, doctors to whom we refer, and, yes, the behind-the-scenes dental lab technicians.
Related reading:
- The crown the lab made doesn't fit: Why does this happen?
- Top 5 questions you should ask a lab before you sent them a case
Any work that is outsourced to a laboratory warrants good communication to those individuals who inevitably make us look good. It’s not easy being a lab technician, though, because just like in any profession, success comes by wading through the muddy waters to get to the other side. I know what makes my job as a dentist hard, but do we doctors know what makes a lab tech's job challenging?
Although I had an idea in mind, I thought I’d go straight to the source to find out—a dental lab technician Facebook group that is 15,000 strong where I posted this question:
I need your help...I’m writing an article that basically goes over the things that we as dentists do (or don’t do) that make YOUR job difficult; i.e., poor impressions, incomplete lab slips, cases you get that more or less make you shake your head. It can be anything. I’d like your perspectives—cut-and-dried—with no sugarcoating.
Whoa. This group is an active bunch, and I have to tell you, I am absolutely appreciative of them for giving me their side of the story. I learned so much and have gained a greater understanding of what it’s like to be in their shoes. In my efforts to improve the status quo for us, them, and ultimately our patients, I’m giving you their answers in raw form so you can see for yourself how challenging their jobs can be! Keep in mind that these are the consistent things that they come across. I have to tell you—we can do better. I’m not saying that everything we send to the lab is bad or horrific, because the technicians absolutely love it when they are able to fly through a case and all we have to do is “drop it in the mouth!”
So, here you go...enjoy!
Disclaimer: There were a lot of comments. Many cover similar topics but from different perspectives. I urge you to read them all.
Clinical challenges
Making good impressions, lab slip instructions, large cases, material usage/choices, occlusal reduction/clearance...
• Leaving cotton or retraction cord in impressions
• Not using retraction cord
• Pouring opposing models in buff stone
• Bad soft-tissue management and a lack of overall general understanding the implant device and its longevity in the given circumstance. Also, lack of tissue adaptation before final prosthesis fabrication
• Impressions! Minimal to no pull if possible. Proper impression tray for size of case.
• Implant placement not ideal but still having to meet the expectations of the dentist and patients; sending stock instead of custom abutments
• Photos are a great tool of communication that are highly underutilized. Don’t use your phone to take pictures! Shade tabs and an in-focus picture of the adjacent teeth and a full face with a natural smile photo can go a long way in ensuring consistent quality of the final restorations.
• No or non-specific instructions or directions given for large cases
• Poor bites on cases with many prepped teeth; no study models or pictures for anterior crowns. • Unreasonable expectations with low-quality impressions, preps to work with. Rushing cases with high-quality expectations.
• New favorite: Doctor sends a digital case with margins marked by someone in their office. They then send the case back saying, “Margins marked incorrectly, remake at no charge!”
• When a digital case is sent and the margins aren’t marked and they expect you to mark their impossibly terrible prep and scan!
• For the love of God, why can’t I get a scan with the correct bite?!?
• Suggestion for docs: Take bite prior to numbing the patient while they’re sitting up
• One of my favorites are free-end bridges impressed with quadrant triple trays or only a quadrant scan—with NO bite!
• Getting all the information on the lab script is always a plus
• Try prepping the occlusal more! Thin restorations fail. To not use those scrappy tin trays that bend.
• Never forget bites and the smile line! Take a small amount of extra away at the margins when prepping.
• Another challenge is accurate bite registrations, or accurate slur/distortion free models that include accurate landmarks and enough teeth that will allow accurate articulation. Many times, the model will be accurate in the prep area but less focus and attention is given to the distal of the posterior teeth. That can have a detrimental effect if it distorts the bite relation.
• Sufficient occlusal space is probably on of the most common challenges we face daily, followed by unreadable margins
• Path of insertion, or draw problems with bridges that occasionally require communication to solve the problem.
• The proximal walls of the adjacent teeth that occasionally tilt toward the prep can make creating a good proximal contact difficult because of the path of insertion.
• Material selection has become much more challenging because of the many options available. It is helpful to communicate to know what end results are desires. This aids in material selection! If you’re unsure, give the lab parameters to make the choice.
• Retract tissue!!!
• Having an exact copy of old dentures so expectations are clear for final prosthesis.
• Only getting minimal clearance and expecting a no charge remake after grinding on a crown that was already at minimal thickness
• Doctors taking a midline on a bite rim when the patient isn’t directly in front of them—they do it sideways in the chair and then try to mark it; it usually results in a bad mark and probably a reset.
• Please take a shade BEFORE you prepare the teeth. During any clinical procedures, teeth dehydrate and this can alter the shade dramatically.
• Not enough room in the bite to make an emergency flipper that will last for more than a week.
• Assuming that teeth can be added to partials all the time
• When evaluating your impression, make sure to capture all teeth/all surfaces of the prep completely.
• I’ve see single centrals that only captured the incisal 1/3 of the adjacent/remaining teeth. It’s difficult to evaluate texture, emergence profiles, etc. Same with posteriors—this severely affects occlusion.
• Use sufficient impression material; some cases may require a custom tray.
• Prep or impression is insufficient. It’s tough to get a doctor's team to nail both of them inconsistently.
• If you do removable in your office, know what a maxillary anterior alveoloplasty is and do it. Also, determine the skeletal class of your edentulous patient and don’t ask your lab to change it ... it sets both of you up for failure.
• We need enough space for material thickness and strength; 1 mm always.
• With modern materials, we need better than a knife edge margin and no sharp angles on the prep—slightly break those sharp edges! The prep should look like a tooth but smaller—molars aren’t flat occlusally ... we need space for a central fossa, perhaps a cingulum and a nice facial incisal-gingival curvature. Pretty straightforward basic concepts.
• Make sure your patient doesn’t bite into the tray while taking the final impression! This leaves pull and distortion, which make the final restoration unpredictable.
• Be aware of manufacturer recommendations and material limitations.
• Making a lateral or cuspid with a quadrant impression and having no idea what the other side looks like and then having the case sent back because it didn’t match the shape/size of its opposite.
• Incomplete information on dockets—i.e., sex, age, shade, date, instructions, stages, missing midline, smile, canine lines, rims trimmed to determine incisal length, teeth removed from try-ins for a new bite.
• I would estimate that about 50% of our Rx’s have something missing: shade, photos, date, implant size, etc. Our doctors are awesome, but it makes for so much extra work.
Communication challenges
Understanding one another, concerns with reciprocating respect and time ...
• Poor case planning
• Having to talk to the assistant rather than the doctor
• Rush cases with unrealistic expectations
• Waiting for dentist to order implant parts yet they still want the case on time
• Lack of mutual respect
• Doctors not understanding the digital workflow or importance of incorporating it
• Communication!
• I love it when an office calls and preschedules so we have enough time to do it right. Hard to rush perfection!
• Accountability (or lack thereof)
• Tech’s conversation with a dentist doing quad impressions with bridges: “She said she has been practicing dentistry for 26 years and knows what she is doing ... I said OK, cool, but I charge for remakes where I have warned you about something.”
• One challenge is when the dentist sends a case to the lab that requires communication, has a due date, but the doctor is too busy to take a phone call, or reply back quickly, which increases the pressure of the time demands of the case. I appreciate being able to send text/email and photos for communication directly to the dentist—IF there is a quick response!
• Losing pride of good craftsmanship when competing with larger labs—get a small lab with some heart.
• Getting a case back from two years ago and asking for a remake at no charge with no explanation!
• Communicate! Dentists love feedback on their abilities too!
• Communicate with our lab (that goes both ways), take us to your CE with you.
• Pay your bill with a credit card on the first of the month.
• To be a successful dentist, you must consider your lab a team member … ask them for their input, especially on treatment planning.
• If your office staff calls to schedule “x” and “x” is a same-day process (simple hard reline/repair), don’t get upset with us when we have to call and tell you that “x” is really “xyz” and will take a couple days. Make sure your staff is forthcoming about what we will be doing so we can give you an accurate turnaround time. Your lack of information and planning does not constitute an emergency on my part.
• Payments on time = respect for me (don’t put me last on the list)
• Be kind to local labs and send some of the difficult cases to them, not just to the labs overseas.
• When we call the doctor for a new impression and we get the answer, “Difficult patient, do your best.” We always do our best but we are not magicians.
• Stop rushing cases, don’t try to negotiate lab fees and pay when a technician comes for a consult with a patient.
So, there you have it. Unfiltered, uncensored, and straight from the mouths of our teammates. Honestly, I’ve been guilty of a lot of these things over the last 14 years, but I have come to know that ultimately, the buck stops with me. I know what’s good, what isn’t, and I can’t blame the lab when clearly the fault lies at my doorstep. I also would submit that lab technicians as a whole really respect their doctors and want them to succeed! When we succeed, they succeed! They do get a lot of amazing cases and good quality things from us, but there is always room for improvement.
I’ll leave you with one last comment from a lab tech that really hit home with me—it’s true in so many ways. Gratitude goes along way ...
Calling the lab when they have done a good job and not just with the problems. Dentists need to realize that lab techs are an important part of the dental team—we are dependent on each other to be successful in this business. We all want to do great work and improve where we are weak. I agree, communication is key. We normally do not get to see the patients and we rarely ever get to know if a case has went well after we have sent it out with a prayer.
About the Author
Stacey L. Gividen, DDS
Stacey L. Gividen, DDS, a graduate of Marquette University School of Dentistry, is in private practice in Montana. She is a guest lecturer at the University of Montana in the Anatomy and Physiology Department. Dr. Gividen has contributed to DentistryIQ, Perio-Implant Advisory, and Dental Economics. You may contact her at [email protected].