The trek to positive polishing: Mastering the challenge to actually use air polishers
By Shirley Gutkowski, RDH, BSDH, FACE
Years ago, as a brand new and substitute dental hygienist, I came across a very odd-looking machine — an air polishing unit. I had no idea how to approach it.
It intrigued me a bit, because I did not like having my teeth polished with gritty prophy paste. Having a little bit of machine know-how and the fearlessness of someone immersed in learning (I was still new, remember) I sought out the directions for using the polishing unit.
-------------------------------------------------------------------------------------------------
- Consider reading other articles by Gutkowski
- How do you prepare for a life-changing event, such as Doc's retirement?
- The New World
- An in-depth view of oral probiotics
------------------------------------------------------------------------------------------------
Thinking back, the first thing that turned me off about air polishing was the sodium bicarbonate polishing compound. It wasn’t that baking soda itself was bad, just that baking soda tasted salty, and that meant I had to ask every person if they were on a sodium-restricted diet. I wondered how problematic sodium bicarbonate is to a person on a salt-restricted diet. I had no idea. I looked at that machine as, what we call in the business, a PITA (pain in the a--). I found time to read the directions, fired it up, and freaked out when it sent out a plume of sodium bicarbonate. The stuff got everywhere, and I tucked the idea of air polishing into a dark corner of my mind.
Not too much later I got a long-term assignment at an office with an air polisher, and someone in the office knew how to work it. So, during one of the downtimes, I polished up a bunch of pennies, and it was cool! By polishing pennies I learned how to manipulate the tip, and how far or close I needed to be to the penny to get off the dreck. This also taught me that the mess could be controlled. I started to ask people if they were on a sodium-restricted diet, and if they weren’t, I used the air polisher on various people with teeth stain. Becoming good at air polishing was hard because not many offices had the machine.
I worked as a substitute RDH for three years before settling down to one full-time office. That doctor didn’t have an air polishing unit, and I practiced traditional polishing with the mildest grit paste I could find. For the five years I was there, I mixed coarser grit for the patients who presented with heavy stain that I couldn’t budge with a sharp hand instrument.
Not until I moved to another office where the air polisher sat unused and wanting to become part of someone’s — anyone’s — dental hygiene appointment protocol, did I take the challenge.
The doctor took the hygiene team to a perio class that stressed air polishing as part of the treatment sequence in people with periodontal disease. Turns out that bicarbonate has a medicinal property. Sodium breaks down bacterial cell walls and helps in reducing edema, and the bicarbonate has fleeting soft tissue benefits. After periodontal therapy, the air slurry polish can make the mouth look like the aftermath of a bar fight. That clears up quickly, and the tissue responds beautifully. In days gone by, one quadrant of the mouth was treated a week or two apart, and the bicarbonate treatment acted as a medicament in the days before Actisite. Remember those days? Three of us were told to share the air polisher, but it became apparent after weeks of moving the machine to my room from the central location for every patient that the other two hygienists didn’t like to follow that protocol.
Since it was a pain to move for each patient, the machine ended up living in my treatment room. I learned to bend and hook the saliva ejector into the patient’s mouth so the tip was free of the oral mucosa, sucking up a good amount of the resulting aerosol and collected water. Patients loved it because the entire procedure was short — less than two minutes. Also, they loved the clean feeling without the grit.
The polishing unit was the size of the Milwaukee telephone book circa 1992. The mechanics of the powder bowl were tricky and it was difficult to keep clean. I had someone come from the company that made the unit to teach me how to keep the system clog free. The bowl was emptied every night by opening up the housing, fishing out the powder bowl, opening it, dumping the powder back into the powder container, spilling some, getting the high volume suction out, vacuuming up the spilled powder, putting the vacuum tip over the little tube in the center of the bowl, hitting the button of the machine to blow out all the tubes into the vacuum system, then carefully managing the bowl back into its spot inside the machine without pinching any of the tubes that fed the air to the bowl. I managed to clog up only one tip beyond repair.
Years and thousands of polished teeth later, maybe even millions of teeth later, I learned more about this unique polishing method and some important benefits, for instance, readying the teeth for sealants. Other than the soft tissue benefits, air polishing had been identified as a major player in sealant placement. In the 1990s, Dr. Gordon Christensen’s group (Clinicians Report) evaluated dental sealants and found that they fail because clinicians do not prepare the tooth correctly. At the time, air abrasion was just starting to come into vogue, and the suggestion was to use the air abrasion before etching the tooth, or at the very least, polish with air/water bicarbonate slurry.
Air slurry polishers are not cheap, and in an effort to “comply” with the bicarbonate treatment before etching, some practice managers/owners suggested polishing with a prophy brush and bicarbonate of soda with a little water. They mistakenly thought that the bubbling of the bicarb was the action they were looking for. It is flawed thinking to convince oneself that if one thing is true, any part of the truth is as good as the whole truth. This is kind of like a patient telling me that flossing once a month is almost as good as flossing once a day. What was supposed to catch on was the air slurry polishing idea, not the bicarbonate idea.
Of course, bicarb is an acid buffer, so etching twice was recommended after a bicarb treatment, and then we added another step to an already complicated process, so the whole thing never caught on. Any sealant was better than no sealant was the feeling. That turned out to be dead wrong, and many teeth have been lost to improper tooth preparation before placement of a resin sealant.
In the early 2000s, bicarbonate was replaced with calcium carbonate. No sodium! It was great for stain removal, as good as the bicarb. We removed the biofilm from the pits and fissures, and all was right with the world. But wait. People like a good taste in their mouth, so next came flavored powders.
Then came changes in polisher designs. The telephone book–sized box of the polisher on the counter, along with the scaler, microscope, and irrigator, took up too much room. Add that clutter to the hoses, wires, loupes, and headlights, and treatment rooms started to become so crowded that finding room for a patient was nearly impossible.
Sleek air polisher designs have the powder and mechanics in the palm of the hand. Doing this makes weight and balance important. The small muscles in dental hygienists’ hands are already taxed, which makes this design a great looker but questionable from an ergonomic standpoint. The number of hoses and wires was reduced, but a little flexibility was lost, and visibility was still problematic.
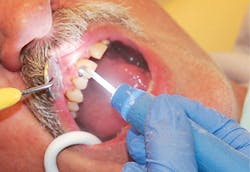
Figure 2
One way to increase visibility is to clear out the debris faster, and a number of suction tips can do that. Crosstex has a new saliva ejector tip that is very tissue friendly and doesn’t need an adaptor. Other companies make vented high-speed evacuator tips that work great, but require a second pair of hands (see Figure 2). Evacuation is great, and when used correctly, the suction also removes the aerosolized particles. Not all though. Part of the beauty of the new powders, particularly the NovaMin particles, is that they’re heavy and don’t fluff as much as bicarbonate. Calcium bicarbonate is also a little heavier than sodium bicarbonate, but the fluff is still there. Evacuation, of course, doesn’t address the last problem with visibility, which is darkness.
Figure 3
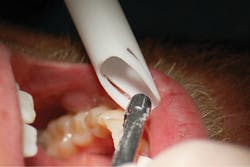
Getting light to the inside of the mouth is pretty easy. Many companies are in the headlight business, and wearing loupes also increases light to the eye. Some air polishing handpieces have a lighted tip, and one cannot argue with the improved visibility (See Figure 3).
The light on the forehead is awesome, but it shouldn’t dissuade a user from investing in a lighted handpiece. Having light where you’re working is the only way to do your work well. The new Suvi combo unit from Coltene/Whaledent is two units in one. The Suvi combo is sleek and easy, and has two lighted handpieces. One side has a top-of-the-line piezo scaler handpiece, and the other is an easy-to-maintain air polishing handpiece. Both have LED headlights!
The polishing compound is a nonsodium-based powder that removes stain and biofilm. The powder is attached to the outside of the unit, where it’s easy to reach and make adjustments. The silicone handpieces are thick and ergonomic. They are also autoclavable. The cords are lightweight and offer very little resistance. The Suvi unit is clean and has a very small footprint on the counter. The foot petal controls power. The dual powder controls are on the foot petal and the powder container. One feature I wasn’t expecting is the ergonomic aspect of the light. Because I can see, I can sit more upright, which makes it more difficult for splash and splatter to hit my face. Bonus!
Another bonus was something I hadn’t seen on other air polishers — a button for cleaning the powder out of the tubing between patients. Seven seconds of pure powder removing powder. I just hold the tip into the patient chair cover or high volume suction and let ’er rip.
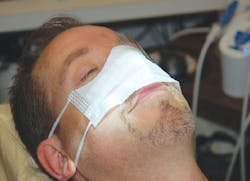
Figure 4
If you’re worried about your patients breathing in the polishing compound, make sure your suction is working. Crosstex makes a patient mask that covers their nose and has an eye shield incorporated into the mask (see Figure 4). The polishing tip design of the Suvi is such that the powder and water are delivered separately until they reach the tooth. This feature allows for better stain removal. Imagine a bull’s-eye where the powder comes out of the center and the water comes out around the powder, reducing the plume.
In short, air polishing is a preferred method for polishing teeth. Patients love it and are happy to forego the grit of the pumice-based pastes that scratch enamel and esthetic restorations. Air polishing is a very important part of tooth preparation in sealant procedures. If you’re not using an air polisher or air abrasion unit before placing sealants, stop placing them. And, just like your first day polishing teeth in your school’s clinic, you’re not going to master air polishing on the first day. Give yourself time to learn how to hold the mirror to protect the tissue and create a barrier. Really, your patients will be appreciative. RDH
SHIRLEY GUTKOWSKI, RDH, BSDH, FACE, is a clinical dental hygienist. Her experience and free thinking have made her a popular international speaker and award-winning author. She is the author of many books, chapters, and articles to support dental hygienists, and she is a career coach at CareerFusion. Her books can be purchased through www.rdhpurpleguide.com. Information on CareerFusion is at www.Careerfusion.net.