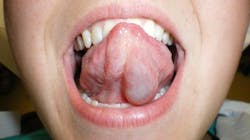
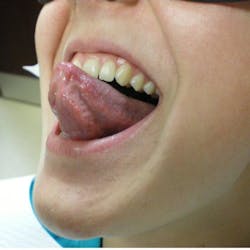
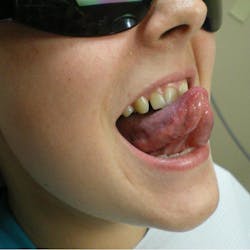
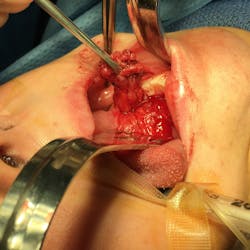
An asymptomatic, fluctuant mass with a bluish hue
Editor's note: Originally published in March 2016. Updated May 2023.
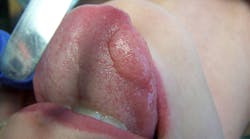
A healthy 21-year-old female was referred by her primary-care physician to my office for evaluation of a “lump” under her tongue that had been present for about two months. The lump had been very slowly growing, totally asymptomatic. The patient said she noticed it “popped” at one time, but it came back a few weeks later. Her physician thought it merited a further evaluation from a dental professional.
The physical exam showed a 2.5 cm painless, fluctuant mass under the left ventral portion of her tongue. There were no other oral lesions present and no cervical lymphadenopathy. The patient’s dental exam was normal as well.
More path cases:
Differential diagnoses
- Ranula
- Mucocele
- Benign or malignant salivary gland neoplasm
- Lymphangioma
- Oral lymphoepithelial cyst
Definitive diagnosis: ranula
A ranula is a lesion that belongs in the category of “mucous escape phenomenon,” which also includes mucoceles and sialoceles.1,2 The underlying problem is not one of a cellular pathologic condition, but rather a problem involving tissue trauma overlying a salivary excretory duct and subsequent healing in a malposed position. This subsequent healing of the duct in an incorrect position causes mucous to be extravasated into the oral tissue rather than the oral cavity. The clinical appearance of this phenomenon is typically that of a painless, fluctuant mass that is often translucent, causing it to have a bluish hue.
Ranulas can range in size from small-diameter masses, like that of the CPC presented in this case, to large masses that extend out of the oral cavity. If the damaged outflow tract is posterior to or through the mylohyoid muscle, ranulas can extend into the neck rather than the oral cavity and cause a phenomenon known as a “plunging ranula.”
Treatment for a ranula, in most instances, requires removal of the offending gland, which is the sublingual gland.2 It has been described to attempt a marsupialization of the fluctuant mass, but is typically met with recurrence of the ranula at a rate of approximately 75%. A correct removal of the gland is a safe procedure with a very low risk of postoperative complications. Removal of the sublingual gland is well tolerated with almost all patients unaware of the reduction in mucous output.
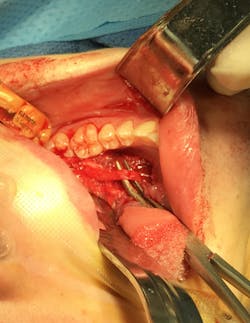
In this case, the area was biopsied given how far onto the ventral tongue the mass lay (most ranulas present on the floor of the mouth), although during the biopsy there was a very easily discernible tract extending inferior to the sublingual gland. The biopsy expectedly returned as a ranula, and the patient was taken to the operating room for removal of the gland. Correct removal of the sublingual gland requires identification of the submandibular duct (Wharton’s duct) and the lingual nerve, which dives under the duct at the posterior extension of the gland. This patient did very well, and the ranula resolved following removal of the gland.
References
- Sapp JP, Eversole LR, Wysocki GP. Contemporary Oral and Maxillofacial Pathology. Mosby; 1997:320-323.
- Marx RE, Stern D. Oral and Maxillofacial Pathology. Quintessence; 2003:511-515.
About the Author

Kevin J. Connor, DDS, MD
Kevin J. Connor, DDS, MD, has a BS in biomedical engineering and earned his DDS degree from Marquette University School of Dentistry. He completed medical school at the Louisiana State University Health Sciences Center, followed by a one-year general surgery internship. He did his oral surgery training in 2010 at LSU and is currently in private practice outside Milwaukee, Wisconsin. Dr. Connor’s surgical interests include dentoalveolar trauma, reconstructive surgery, and surgical treatment of temporomandibular joint diseases.