Why phasing restorative dental treatment can be helpful for both dentists and patients: A case study
Payment plans often become the topic of conversation when a patient's dental treatment plan involves a sizable amount of restorative dentistry. Cost can be one of the biggest factors preventing patients from accepting the dental treatment they need. Dr. Zachary Sisler presents a case study to illustrate the benefits that the underutilized concept of phasing restorative dental treatment can offer to both patients and dentists.
Editor's note: This article first appeared in Breakthrough Clinical, the clinical specialties newsletter created just for dentists. Browse our newsletter archives to find out more and subscribe here.
“WHAT TYPE OF PAYMENT PLANS DO YOU OFFER?” This is a common question heard in many dental offices, especially when a patient’s condition requires a sizable amount of dental treatment. It’s no secret that cost can be one of the biggest factors preventing patients from getting the care they need.
There are several monthly payment options available on the market today, such as home equity loans and plans from third-party independent financing companies. However, these offers may not always be in the best interests of the patient or the dentist. Some of these options require dentists to incur a large fee by accepting independent financing payments, and patients are often charged extra interest fees simply because they are not able to afford all of their dental treatment costs up front.
What if there were another option out there for patients? What about something where dentists and patients were able to work together to formulate a solution to meet their needs as well as their budgets? One great way that is underutilized is the process of PHASING RESTORATIVE TREATMENT.
If it were possible for restorations to be completed in multiple phases, patients could afford dental treatment in smaller increments. This could reduce the need for both patients and dentists to pay excessive origination and interest fees required by independent finance companies.
For example, a patient presents needing $20,000 worth of treatment but can only afford $10,000 at that particular time. The task now falls to the dentist to find a way to phase the treatment while maintaining a biologically and functionally stable patient. When the phased option is presented to the patient, he or she is able to accept it and able to afford it. The patient is also aware of the expected future treatment and associated costs.
With phasing dental treatment plans, dentists can improve the function and esthetics for a patient while still managing the patient’s time, emotions, and monetary constraints.
Understanding the potential reasons to phase dental treatment
It’s important to consider the reasons why a patient may be hesitant to agree to comprehensive or restorative treatment. These reasons need to be acknowledged and brought to the forefront of the treatment planning decision in order to ease the patient’s mind and gain his or her trust.
Physical—
Some patients may be physically unable to sit in the dental chair for extended periods of time. Temporomandibular joint (TMJ) and back issues may make extensive work in a single visit uncomfortable and cause the patient to be hesitant to go through with treatment. In this case, the goal should be to have shorter appointment times to alleviate the patient's concern. Explain to the patient that it is acceptable to take multiple breaks during appointments. This can reduce any stress the patient might be feeling.
Emotional—
Many patients are self-conscious about their teeth, especially those who want and know they need esthetic changes. Easing into these conversations and approaching the topic delicately can begin to eliminate some of the anxiety these patients have. By phasing the treatment plan, the patient will be able to slowly build confidence and feel more comfortable committing to more work as the treatment progresses.
Mental—
Some patients cannot or do not understand the need for their dental treatment. Helping educate them about the consequences of issues going untreated might begin to open doors of opportunity. It often helps to have a spouse, family member, or friend join such patients when discussing the treatment plan. The dentist can educate the patient and his or her trusted source on the risks of not going through with treatment, and then also show the reward of taking action through discussion of similar successful cases. Having someone act as a sounding board can help provide clarity for the patient about the treatment plan and the potential for a positive outcome.
Financial—
Money is likely the most common barrier to receiving treatment. Patients may feel that the treatment is simply too much to afford all at once. The best question a dentist can ask is, "What does your budget allow for right now?" Many times, a dentist can find room to work within the budget, and this will allow the patient to feel financially comfortable while receiving the needed treatment.
The bottom line is that phasing restorative treatment can break down barriers and allow patients to get the treatment they need and desire.
Communicating the dental treatment plan to patients
Having an open line of communication between the dentist and the patient is a key component to gaining treatment acceptance. Expressing concern and letting the patient know the consequences of inaction can help ease concerns and open the patient's mind to the reality of the situation.
For example, the dentist could say, "Mrs. Jones, I’m starting to see some wear on your teeth. If you want to keep them for a lifetime, we might need to talk about a plan for treatment in the near future." This simple statement has two key points: (1) the dentist recognizes and communicates the fact that the teeth are beginning to breakdown, and there could be potential consequences if nothing is done to remedy the situation; and (2) it puts the responsibility back on the patient to take action.
Communicating from a standpoint of true concern establishes a foundation on which to build treatment plans when patients are ready to accept them. It must be understood, though, that due to the cost of some comprehensive treatment plans, patients may need help in becoming ready and willing to pursue solutions for their issues. This is why having the conversation up front about patients' time or monetary constraints is a necessity. These conversations can save time and frustration for patients and dentists alike.
Phasing restorative treatments: Biological versus functional
The goal of any treatment plan is to promote long-term stability for the patient. The success of a treatment plan hinges on the dentist’s ability to examine and diagnose two key components of a patient’s overall oral health: biological and functional. Recognizing the components and maintaining stability in each phase is the only way to ensure a long-term, predictable result.
Biologically, a patient may have systemic issues, such as medications that cause dry mouth, airway issues, hypertension, diabetes, or other illnesses that need to be treated by a physician. Dentally, the patient may have periodontal disease, caries, or abscessed teeth that require additional treatment. This component is often what is taught in dental schools across the nation.
Functionally, a patient may have TMJ issues with joint or muscle pain, wear, mobility, migration, or broken teeth. The dentist must determine the potential risk factors and causes of the functional issues to determine the best plan of action. The functional component generally goes beyond basic dental education and training.
It is important to understand that the dentist should not have a singular focus on either biology or function. The two concepts are intertwined and must be treated together with proper plans for phasing restorative treatment.
To manage the functional component—which will be demonstrated in the case report that follows—it is absolutely crucial to establish and maintain a sound occlusal scheme. There are five requirements of occlusal stability that need to be met and treated in order to stabilize a patient for the long term:
1. Stable and equal intensity contacts on all teeth coinciding with centric relation (CR)
2. Anterior guidance in harmony with the envelope of function (EOF)
3. All posterior teeth disclude during mandibular protrusive movement
4. All posterior teeth disclude on the nonworking side during mandibular lateral movement
5. All posterior teeth disclude on the working side during mandibular lateral movement
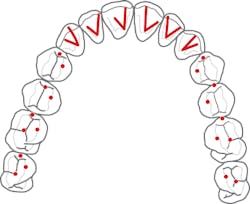
To summarize the five requirements of occlusal stability, see the illustration with lines in the front and dots in the back (figure 1).
Figure 1
If any one of the five requirements of occlusal stability is not fulfilled, the occlusion is considered to be unstable unless the patient has a substitute for the missing requirement, such as a tongue thrust in place of anterior guidance, or the patient has eliminated the need for the missing requirement, such as a Class III skeletal growth resulting in a more vertical chewing pattern.
When talking about phasing restorative treatment, or even with a smaller treatment plan, dentists cannot ignore the signs of instability and expect to achieve a long-term, stable result. A key component from a functional standpoint is fulfilling the five requirements in each phase. The patient can then return when ready to accept more treatment and still be stable throughout the phases of treatment.
Case study
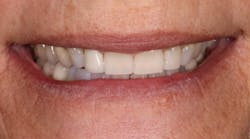
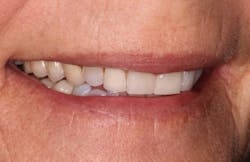
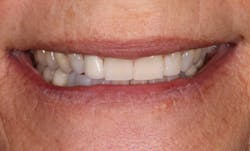
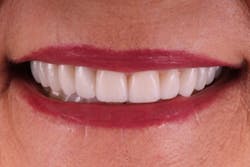
When patients are able to phase treatment and are happy with the results, they are happy to talk about their experience. "Janet" was a current patient of record and had seen a friend's recently completed smile transformation. When Janet came in for her routine periodontal maintenance appointment, she inquired about potential options to esthetically change her smile (figures 2–4).
Figure 2
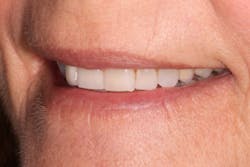
Figure 3
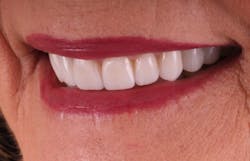
Figure 4
Janet was alternating recall appointments between her general dentist and local periodontist. Therefore, when analyzing her biological component, the periodontist was consulted. It was determined that Janet's periodontal disease was at a stable and maintainable state, and she was clinically ready to move forward with further treatment.
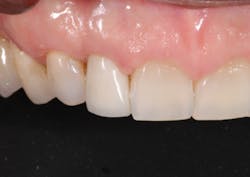
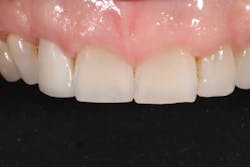
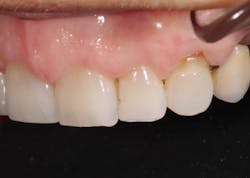
Janet’s chief complaint was that her teeth were starting to wear and become shorter. She also had multiple shades from preexisting crowns and bridges, and overall, she felt that her teeth were flat and lacked definition (figures 5–7). Additionally, there appeared to be signs of functional instability that needed to be addressed. All of this was explained to Janet and a comprehensive, full-mouth treatment plan was discussed.
Figure 5
Figure 6
Figure 7
Janet was hesitant, as many patients are, due to the scope of treatment and cost. After discussing her goals for her smile and the financial considerations, she decided she wanted to focus on her maxillary teeth first. With this new set of parameters, it was determined that treatment could be broken down and phased over two to three stages in order to reduce the initial up-front cost. These were the treatment plan phases:
Phase 1: Equilibration, crowns Nos. 3–14, composite bonding Nos. 22–27
Phase 2: Veneers Nos. 21–28
Phase 3: Crowns Nos. 20 and 29, implant crowns Nos. 19 and 30
The key thought process was that once the function and esthetics had been established for the upper arch, the lower arch could be completed one tooth at a time or several all at once. Having established and maintained the five requirements of occlusal stability, the lower-arch treatment becomes very routine and predictable dentistry.
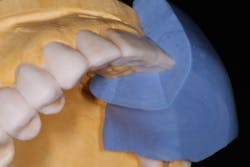
For phase one, a diagnostic wax-up for the maxillary arch was completed. The wax-up serves as the blueprint for the newly desired esthetics and function. In trying to achieve anterior guidance in harmony with the envelope of function, the lingual contours of the maxillary anterior teeth are waxed up to ideal contours. This can then be transferred to the preparations using a silicone prep matrix and tested in the corresponding provisionals (figure 8).
Figure 8
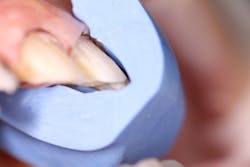
During the first appointment, the lower incisal edges of teeth Nos. 22–27 were bonded with composite to restore the worn tooth structure. This was followed by preparation of the teeth for all porcelain crowns from teeth Nos. 3–14. The prep matrix was utilized to ensure proper reduction (figure 9). Once the provisionals were placed in the mouth, the five requirements of occlusal stability were established. The patient then tested these provisionals for one week and returned, stating no complaints with any of the esthetics, phonetics, or function. An impression of the approved provisionals was taken and then facebow-mounted in order to communicate all of the information to the laboratory for the final restorations.
Figure 9
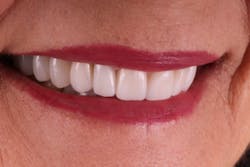
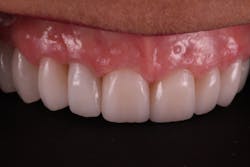
Janet returned to the office to deliver the final restorations and was thrilled with the results. She was officially finished with phase one of the treatment plan (figures 10–12). Her esthetic concerns diminished now with a smile that had every detail she desired, such as embrasure form, definitive line angles, depth of character, and incisal translucency (figure 13). Since her initial concerns of esthetics and function had been stabilized, she would be able to come back and complete phases two and three on a timeline that worked for her. It was stressed that she would need to continue maintenance of the periodontal component.
Figure 10
Figure 11
Figure 12
Figure 13
Conclusion
For patients who are ready to hear or who are actively seeking solutions for their dental problems, phasing restorative and cosmetic treatment could be a gateway for their being able to afford it. The successful completion of phasing treatment is the result of the dentist meticulously examining each patient and determining the potential risk factors that could create a problem in the future.
By paying attention to the details and establishing a stable, predictable long-term prognosis, dentists can begin to break down potential barriers for patients accepting the treatment they need.
Editor's note: This article first appeared in Breakthrough Clinical, the clinical specialties newsletter created just for dentists. Browse our newsletter archives to find out more and subscribe here.