Endodontic case study: referred pain leads to diagnostic uncertainty
Many variables are involved in determining the outcome of root canal treatment. Microanatomy within the root canal and complex interactions within a bacterial biofilm can prevent clinical success even with the most modern treatment protocols. In spite of anatomical variability, success rates for conventional endodontics are high and approach 90% in many studies. However, one way to be absolutely certain of a problem following endodontic treatment is to enter the incorrect tooth.
ALSO BY DR. DAVID LANDWEHR |Endodontic case study: an alternative method for the cleaning and shaping of a mid-mesial canal
Chief complaint: Increasing pain from the upper back tooth on the right side for several days. Pain worse to biting pressure, and cold makes the area feel better.
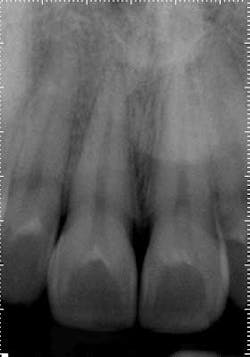
Exam: Teeth Nos. 2 through 5 responded normally to cold with no lingering and were asymptomatic to percussion, so the field of testing was expanded. Tooth No. 8 was nonresponsive to cold and heat. Both Nos. 7 and 8 were hypersensitive to percussion but had no restorative history, and the patient denied any history of trauma. There was no clinical evidence of an enamel defect associated with tooth No. 8. Radiographically, the apical and crestal bone was unremarkable around teeth Nos. 2 through 9. Teeth Nos. 3, 4, and 5 had significant restorative histories.Anterior preop
Pulpal diagnosis: Necrotic pulp No. 8
Periapical diagnosis: Symptomatic apical periodontitis
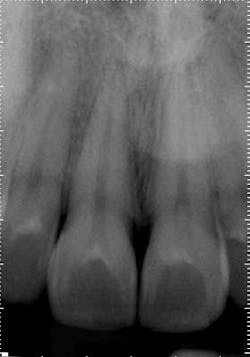
Treatment options: Root canal treatment No. 8, no treatment, or extraction. The patient was certain tooth No. 3 was the culprit, and No. 8 had no restorative or trauma history. As a result, waiting for symptoms to localize was a consideration. However, the patient experienced significant relief following administration of local anesthetic around tooth No. 8, and a root canal was completed.Posterior right
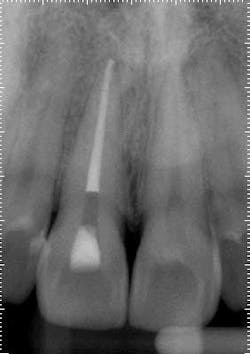
Treatment: Upon access, a necrotic pulp was identified. The dentin triangle was removed with a series of Gates-Glidden burs. Copious irrigation was completed with sodium hypochlorite. The canal was instrumented with stainless steel hand files and rotary ProFile series 29, both 0.04 and 0.06 taper. The canal was filled with a warm vertical downpack and thermoplasticized gutta-percha backfill. To maximize esthetics, the space was underfilled to the level of the crestal bone to prevent staining the chamber.
Although technically a very straightforward root canal, this case illustrates the importance of pulp testing in determining the etiology for pulpal pain. Because of limitations with pulp testing and the potential for pain to refer to distant sites, treating the wrong tooth is a constant threat. Also, it is critical to remember that headache, TMJ, sinusitis, and other disorders can mimic pain of pulp origin.